Are there Endemic Cases of Leprosy (Hansen’s Disease) in Florida?
There are very few new cases of leprosy diagnosed in the US – generally less than 200 people annually – which is far less than the 75,000 cases diagnosed between 2021 and 2022 in India, the country with the highest recorded number of leprosy cases.
Nearly all US cases are attributed to people who acquired the diseases overseas.
However, epidemiologists are concerned about a small, growing cluster of leprosy cases in Central Florida that *may* have become endemic, e.g. capable of being spread locally rather than acquired during travel outside the country.
The Underlying Disease Mechanism of Leprosy
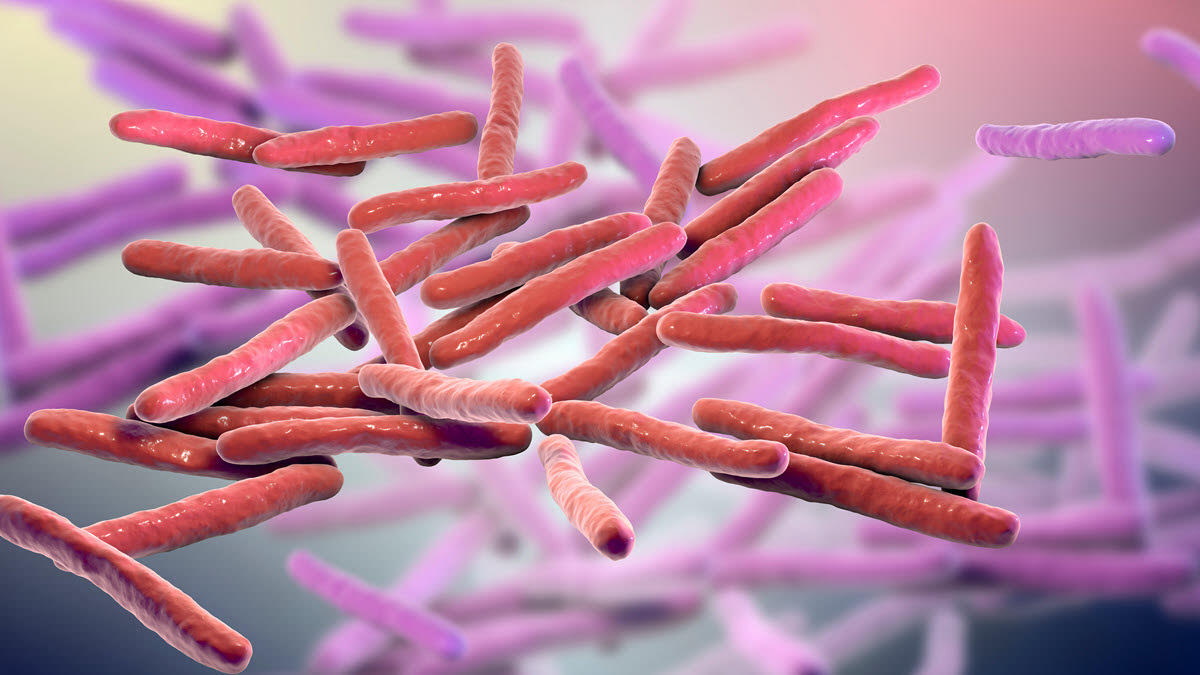
The disease has a long history (it’s even mentioned in the New Testament), but leprosy’s mechanism of disease remained a mystery until 1875 when the Norwegian physician Gerhard Armauer Hansen identified the bacterium Mycobacterium leprae as the underlying cause.
Unfortunately, for centuries, patient isolation was the accepted way to control leprosy’s spread in the population until 1941, when the drug promin (sodium glucosulfone) was found to be successful in treating the disease.
Promin is metabolized as dapsone (4,4′-sulfonyldianiline (SDA) or diamino diphenyl sulfone (DDS), and so the clinical therapy was revised to administer dapsone directly to patients starting in 1945. (Dapson is listed in WHO’s Essential Medicines List (EM).)
Today. patients with less severe cases (paucibacillary leprosy) are treated for 6 months with a triple antibiotic course of dapsone, rifampicin, and clofazimine. More advanced cases (including multibacillary leprosy) are treated for 12 months and may require additional antibiotics.

Clinical Tests for Diagnosing Cases of Leprosy
Leprosy can damage skin and nerves, resulting in instances of thickened and/or scaly skin, a lack of nerve sensation, and in advanced cases, atrophy of fingers and limbs.
Because leprosy cases originating in the US are so rare, most clinical healthcare providers won’t screen for leprosy unless the disease has advanced to the point where skin lesions or other symptoms have appeared (although the CDC recently advised practitioners in central Florida that they should be on the alert for the disease).

After an initial diagnosis is made, a skin smear test is performed to identify the presence of either Mycobacterium leprae bacteria or Mycobacterium lepromatosis, a very closely-related bacteria variant isolated in 2008.

The standard clinical diagnostic test used to identify the presence of the bacteria in the skin smear is the century-old Ziehl–Neelsen acid-fast stain test, in which a highly penetrative red carbolfuschin dye is added to the sample.
Carbolfushin dye can penetrate the waxy, lipid internal structure of so-called “acid-fast” bacillus (AFB), including Mycobacterium, which causes it to turn red. Heat is added briefly to stabilize the dye stain, then an acid solution of ethanol with a small amount of hydrochloric acid is used to “wash” off the stain; however, the acid doesn’t penetrate acid-fast bacteria, leaving the red color intact. To complete the test, a counter-stain of methylene blue is added to the sample, which will ‘re-stain’ the non-acid-fast bacteria, creating easily distinguishable blue and red stains that enable the lab clinician to differentiate between acid-fast and non-acid-fast bacteria.
But you may be asking, can’t we somehow test for leprosy before symptoms appear? Unfortunately, there are no single, straightforward clinical screening tests available for asymptomatic leprosy cases.
This is due in part to the inability of Mycobacterium leprae or Mycobacterium lepromatosis to exist and grow on their own, e.g. in-vitro in a lab petri dish. Instead, they require a live host animal, such as a lab mouse, to propagate.

Laboratory scientists are looking at several options for creating a simple universal screening test for Leprosy, including:
- Test for the presence of leprosy antigen-antibodies, not unlike a rapid Covid test.
- Use a qPCR test to amplify and detect the presence of unique gene snippets from Mycobacterium leprae or Mycobacterium lepromatosis.
- Try to identify some universal biomarkers that would confirm the presence of leprosy; currently, this is difficult due to the varying immune system responses during different disease stages and highly variable individual responses.
- Use an immunochromatographic ML Flow test to detect the presence of anti-PGL-I IgM in human blood or serum, which would indicate an immune response to the Phenolic glycolipid-I (PGL-I) molecule in the cell wall of Mycobacterium leprae or Mycobacterium lepromatosis.
Hopefully, one or more of these research efforts will result in a simple screening test to help identify leprosy infections.

Why Florida? Are there Environmental Reservoirs of the Bacteria that Cause Leprosy?
Leprosy does spread in the environment, but not easily. Contact with those with the disease does increase the risk of transmission, although the overall chances are considered low. Complicating the situation is the fact that many who are infected by Mycobacterium leprae or Mycobacterium lepromatosis remain asymptomatic without any apparent disease progression.
For a long time, it was assumed that direct skin contact was the primary transmission mechanism for leprosy, but more recently, scientists are speculating that aerosolized bacteria are transmitted to the upper respiratory tract, causing infection.
Leprosy patients who are being treated with approved antibiotic treatments (see above) can safely contact others after the first 72 hours of treatment.
So this brings us back to the question, why the small outbreak in Florida?
Could there be a natural reservoir of leprosy bacteria in the environment?
Some point to the relatively large armadillo population in Florida as a zoonotic reservoir of the disease. Armadillos can harbor the leprosy bacteria – but since leprosy was unknown in the Americas before European contact, epidemiologists speculate that humans arriving from Europe originally transmitted the bacteria to armadillos, not the other way around.
Since one of the Florida leprosy patients who appeared to acquire the disease locally was a landscaper working outdoors, the infection is somehow related to contact with armadillos in the wild, although we don’t know for sure.
If there was a simple, inexpensive, non-invasive test it (for humans and armadillos) would be easier for epidemiologists to track the progress of the disease. For now, we have to see what trends emerge.
Support for Neglected Tropical Diseases (NTD)
Within the WHO lexicon of health care, leprosy is considered to be a “Neglected Tropical Disease” (NTD), which helps bring focus and some limited resources toward disease research and treatment. The WHO supports efforts around the world to treat leprosy by offering free courses of medication.

Troubling Cases of Malaria in Florida and South Texas
As the climate warms up, mosquitoes are on the march. Researchers recently discovered mosquito species as far north as Finland that carried tropical diseases.
We recently reported on the science behind malaria vaccination campaigns in Africa, but is it now time to think about preventing the spread of malaria in the US?
The time has come.
In June 2023, the CDC issued an emergency health advisory to alert public health professionals of the possibility of locally-acquired cases of malaria transmitted by the Plasmodium vivax parasite in South Florida and South Texas.
What can be done?
As we reported, anti-malaria vaccine campaigns in Africa are using the R21/Matrix-M vaccine developed by Oxford University (which uses the Novavax Matrix-M adjuvant) and the RTS,S/AS01 vaccine, developed by GSK and marketed under the brand Mosquirix.
These vaccines are incredibly valuable for controlling the spread of malaria but do not provide 100% protection.
Researchers are looking at several promising new anti-malarial drugs that might give greater protections, including:
- The discovery by GSK researchers of the Tres Cantos 1 (TC1) bacterium (a strain of Delftia tsuruhatensis) that inhibits the Plasmodium falciparum, one of the two common parasites that transmit malaria via mosquitoes.
- A vaccine that targets the Duffy-binding protein in Plasmodium vivax, the other common parasite responsible for malarial infection via mosquitoes.
- Research on malaria transmission-blocking vaccine (TBV) candidate Pfs25, which would teach the immune system to recognize a specific antigen necessary for malaria transmission by Plasmodium
- An mRNA-based anti-malarial vaccine developed by researchers in Australia and New Zealand

More Invasive Species on the March: Spotted Lanternflies, Murder Hornets, and Poisonous Hammerhead Flatworms
Environmental and laboratory researchers also have their hands full trying to keep up with invasive species on the march.
· Spotted Lanternflies (SLF)
This invasive insect originated in China but was discovered northeast of Philadelphia in 2014. As of 2022, Spotted Lanternflies have spread to much of the Northeast, creating a serious threat to grapevines, fruit trees, and commercial timber. The insect sucks sap from the trunks and branches of plants, resulting in damage, even death. Unfortunately, the overwintering eggs remain viable unless exposed to very cold temperatures (-13 F), which is becoming less common across the US, given the warmer winters in recent years. Agricultural researchers are investigating if it is safe to introduce foreign predator species that control Lanternfly outbreaks in China, including the eupelmid wasp Anastatus orientalis, which eats Lanternfly eggs.
· Murder Hornets (Giant Northern Hornet)
There was much-wellfounded hysteria in 2020 when giant Asian wasps were discovered in the Pacific Northwest Region. These wasps, commonly known as Murder Hornets, have been officially named the Giant Northern Hornets. Genetic testing revealed the specimens found in the US are derived from a mix of native Chinese and Japanese stock.
Fortunately, in December 2022, the Washington State Department of Agriculture announced there had not been any confirmed sightings of the hornet in the state during the preceding year. However, research continues to identify any outbreaks in the wild as well as evaluate the potential pros and cons of introducing foreign bio-predators to control their spread if they return.
However, we are not out of the wood yet (so to speak). This August, the Georgia department of agriculture (GDA) reported that a beekeeper in Savannah found a live Asian yellow-legged hornet, a dangerous invasive species from Asia that is a major threat to honeybees and has already become established in Europe and the UK.
· Poisonous Hammerhead Flatworms
East Coast residents were surprised to learn that poisonous hammerhead worms (Bipalium adventitium and Bipalium vagum) are migrating northward. These worms range in size from an inch to as much as a foot or more and feature a distinctive double-ended “head” that resembles a hammer. Their slime is potentially poisonous to the touch; it contains a tetrodotoxin neurotoxin that’s similar to that found in certain puffer fish and octopuses. Researchers recommend keeping pets away and avoiding touching the worms. (Use gloves if necessary.) Cutting the worms to kill them is not effective; in many cases, the pieces will regenerate into new worms. Salt, however, is a safe control alternative. Researchers need to gather more data on this invasive species to identify the level of risk they pose to native species. (The Bipalium vagum variety appears to eat snails, which could put native snails at risk.)
Formaspace is Your Laboratory Research Partner
If you can imagine it, we can build it, here at our factory headquarters in Austin, Texas.
Contact your Formaspace representative today to learn more.










